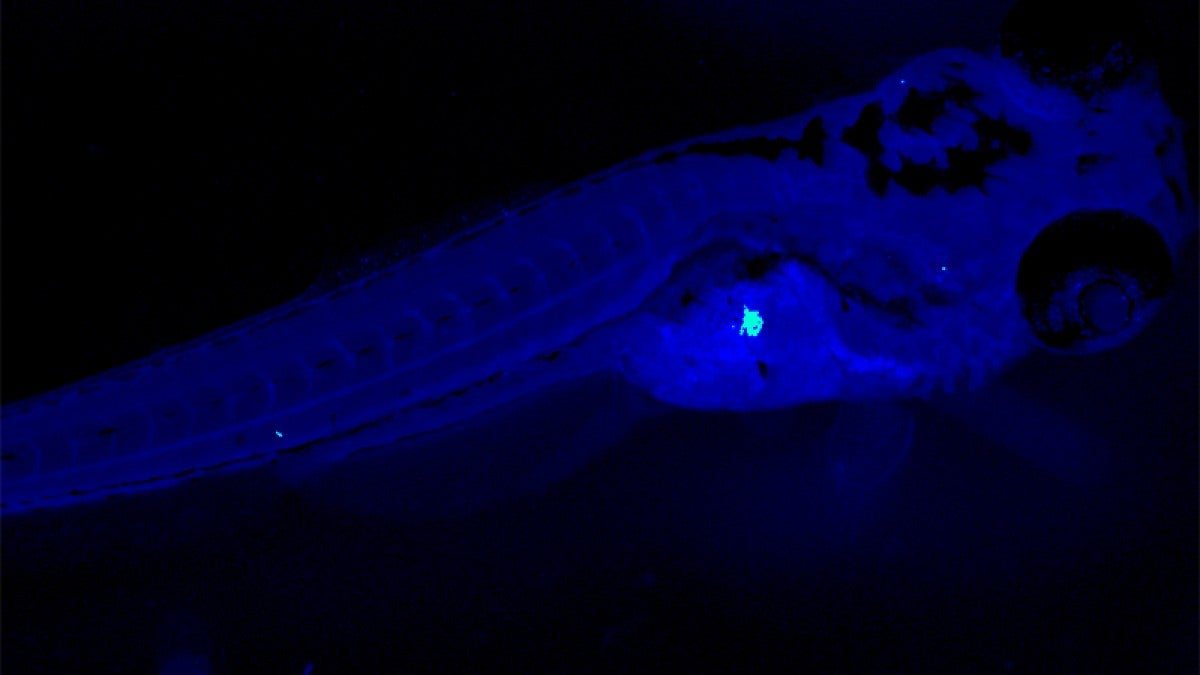
A newly discovered bacterial protein produced in the zebrafish gut triggers insulin-producing beta cells of the pancreas to multiply during early larval development, say University of Oregon researchers.
The research potentially has human health implications. Beta cells are the only cells that produce insulin, a hormone that regulates sugar metabolism. A lack of insulin production is associated with Type 1 diabetes, an autoimmune disease that affects some 1.5 million people in the U.S.

The research demonstrates the developmental role of teeming communities of bacteria and other microbes — the microbiota — in the bodies of animals, said UO biologist Karen Guillemin, a co-author. Understanding how the microbiota affects the development of beta cells, which are lost in patients with Type 1 diabetes, eventually could lead to new diagnostic, preventative and therapeutic approaches for this disease, she said.
“We're realizing that the microbiome is a rich source for discovering new biomolecules that have enormous potential for manipulating and promoting our health,” said Guillemin, a professor in the UO Department of Biology and Institute of Molecular Biology. She also is director of the UO’s META Center for Systems Biology.
Using germ-free zebrafish as a model, lead author and doctoral student Jennifer Hampton Hill explored the possibility that certain gut bacteria are necessary for the pancreas to populate itself with a robust number of beta cells during development.
She found that, during the first week of life, germ-free fish did not undergo the same expansion of beta cells as conventionally reared fish. Exposing the germ-free fish to specific bacteria, however, restored the beta cell mass to normal levels. This restoration became the basis for her search and ultimate discovery of a novel bacterial protein that on its own could stimulate the growth of insulin-producing cells.
Related commentary in eLife: Microbiota: From bugs to beta cells
“The research suggests that animals rely on the cues and signals from the microbial communities that inhabit their bodies and that they are important for very intricate parts of development,” Hampton Hill said. “It’s exciting to think that bacteria could play such an important role in a process that is so essential for homeostasis, for the ability to regulate glucose metabolism.”
“This is a new idea that the microbiome could be a source for signals for the development of the pancreas,” Guillemin said. “This is the first time that anyone has made a connection between the microbiome and the development of beta cells.”
Scientists have been increasing their understanding of how host-associated microbes influence the development of the gut and immune system, but the formative role of microbes in other digestive organs such as the pancreas remains an underexplored area, the researchers said.
The UO has been a leader in zebrafish research since the 1960s when biologist George Streisinger pioneered a new method for the study of vertebrate development and genetics with the introduction of the small fish as a model organism. Over the past 15 years, Guillemin and colleagues have developed methods for growing germ-free zebrafish, allowing them to ask what happens when the animals develop in the absence of microbes.
The use of germ-free zebrafish allowed Hampton Hill to methodically screen for gut bacteria that could stimulate beta cell proliferation. She then focused on one bacterium from this group and investigated its secreted proteins for beta cell-expanding activity. Those efforts led to a list of 163 prospective proteins.
She next turned to the genome sequences of the previously screened bacteria and asked which of the prospective proteins were shared by the beta cell-expanding bacteria and absent from inert bacteria. Her criteria returned only a single protein candidate that had never been studied. When she made a purified version of it and added it to her germ-free fish, the beta cell population expanded — earning the protein its name of Beta Cell Expansion Factor A, or BefA.
Knowing the molecular identity of BefA allowed the researchers to search for its sequence in other bacterial genomes. They found it to be present in several common human-gut associated bacteria. When Hampton Hill purified two of these related proteins from human bacteria, they proved to be equally potent at stimulating beta cell expansion in zebrafish.
“We had spent many years collecting and characterizing zebrafish gut bacteria, and it was gratifying that we could harness all of this knowledge in the discovery of BefA,” Guillemin said.
The finding that specific gut bacteria produce proteins that stimulate beta cell development sheds new light on epidemiological data connecting low-diversity childhood microbiomes with increased Type 1 diabetes risk. It may be, Guillemin and Hampton Hill said, that low-diversity microbiomes are less capable of stimulating beta cell expansion early in life, leaving children with little buffer if their immune systems go on the attack.
An implication of the study, Guillemin said, is the importance of promoting healthy microbiome development in children — for example, by promoting breast feeding and avoiding excessive use of antibiotics.
Additional research is needed to identify the mechanism by which BefA proteins affect beta cell development and whether the proteins have the same effect in other animals, including humans, she said. “Ultimately we’d like to team up with researchers studying Type 1 diabetes to look at developing BefA-related molecules as potential therapeutics.”
Additional co-authors on the study were Eric A. Franzosa and Curtis Huttenhower, both of Harvard University's T. H. Chan School of Public Health in Boston and the Broad Institute in Cambridge, Massachusetts. Co-author Guillemin also is affiliated with the Humans and the Microbiome Program at the Canadian Institute for Advanced Research in Toronto.
The National Institutes of Health supported the research through grants P50GM098911, T32GM007413 and P01HD22486.
— By Lewis Taylor, University Communications