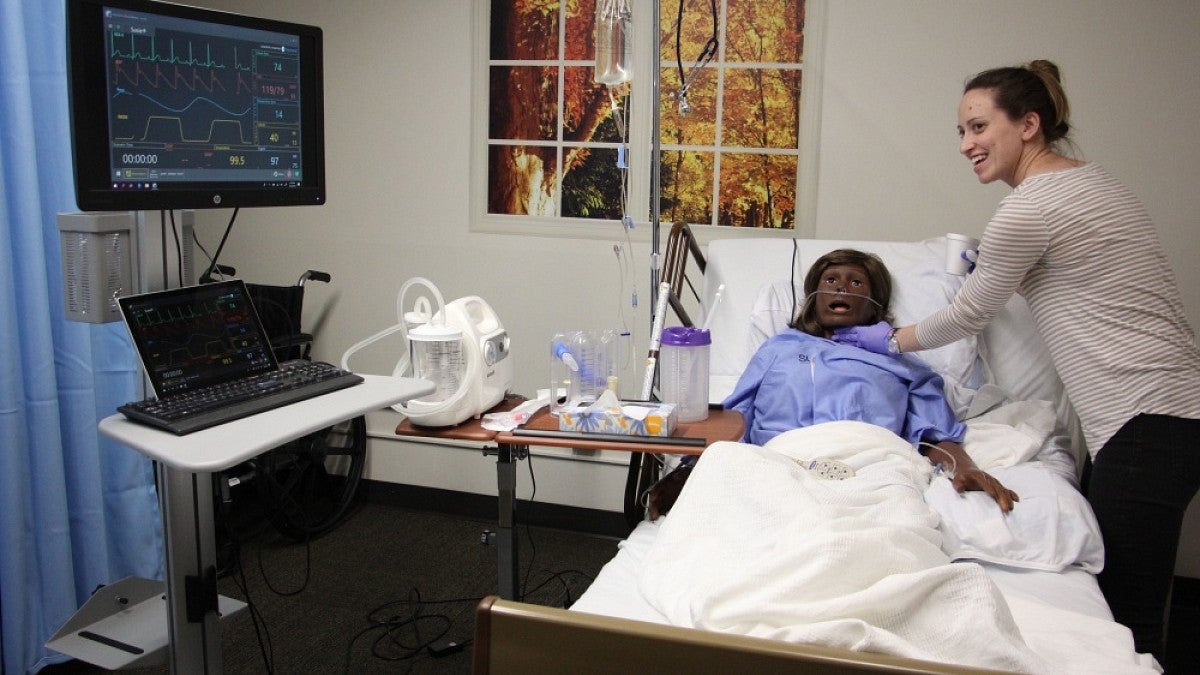
Step through a doorway deep inside the College of Education’s Clinical Services Building and you get the feeling that you have been transported into a hospital room.
A monitor displaying real-time vital signs, an IV bag, tubes, an oxygen tank and other gadgets you’d expect to see in most hospital rooms, along with the rhythmic and random beeps and tones — they’re all there. It also includes a manikin that “breathes,” has a heartbeat and can reply to questions, and that’s where the real learning comes in.
This is the Communication Disorders and Sciences program’s new hospital simulation lab, a place where students in the program can log valuable experience that will prepare them for what they may see in the field. The lab also vaults the program into the same league as those associated with a hospital or similar facility and helps feed sharp demand for a field that is fast growing.
“What’s always been a challenge for us is meeting the needs of medical training in the absence of an academic medical center,” said Samantha Shune, an assistant professor in the Communication Disorders and Sciences program. “We have great collaborations with partners in the community: hospitals, nursing homes. But it’s not like we have ready access to just take students into a hospital room and say, ‘Let’s train you on the sights, sounds and feel of a hospital room.’”
“Simulations in medical training is not a new concept,” added Jennifer Meyer, director of clinical education in the program. “But simulation training in speech pathology in the absence of a medical school is a newer thing.”
Shune and Meyer assembled the lab over the summer, which fills what was a hole in the program’s offerings. Prior to this, students weren’t always going to be familiar with what they might encounter when they first set foot in such a setting. Now, they’ll know the landscape and have some hands-on experience.
What’s more, they would encounter scenarios they were most likely to face in the real world, only they’d come in the supportive, far less stressful environment of the lab.
“The simulation lab is transformational for training future clinicians to evaluate and treat patients in the hospital,” said McKay Sohlberg, director of the Communication Disorders and Sciences Program and graduate program director. “It is remarkable how realistic the scenarios are that you can program. It has truly improved our instruction.”
During fall term, the first group of grad students put the lab to good use in clinical training and as an academic setting, and it received rave reviews.
“Students love it,” Meyer said. “They want more time in the lab, more assignments in the lab. It’s exciting for the students and an incredible opportunity at a place where the stakes are low. The faculty are excited to have this teaching environment, too.”
Students go through the same exact routine they would go through if they were entering a real hospital room, down to washing their hands and checking on and recording vital signs.
The magic happens with the manikin. Either Shune, Meyer or one of the other program’s supervisors sits behind a curtain in the back of the room with a computer that is connected to the manikin. Students get a case history and then follow what would be a standard script they’d ask just about any patient.
Based on survey results from previous alumni of the program, Shune and Meyer designed learning modules around areas that they felt students needed more exposure and experience with. Then they developed several simulations for the manikin and put the students through them.
They also logged prerecorded replies they can make the manikin repeat or they can go off-script and speak into a microphone that makes it sound like the voice is coming from the manikin. They can make it sound like she is struggling to speak or has something caught in her throat. They can adjust the manikin’s vital signs and breathing on the fly as students ask the manikin to speak or swallow, making students decide how to proceed further during the visit.
The room also has an infant manikin for students to work with, although it isn’t interactive.
At the end of the “visit,” they come up with the recommendation they’d give to a doctor.
“We like to emphasize that this is a learning opportunity, not a time to test you,” Shune said. “If you have a question, we can pause to talk about it in the moment.”
Shune and Meyer eventually hope to add in a bilingual component or pull in theater arts students to play the role of a caregiver or advocate the students interact with.
The time in the lab counts toward students’ clinical hour requirements, and those in the clinical program spend a couple hours in the lab each week learning things they would need to be able to do in an inpatient acute care setting.
“They’re getting to come into this setting, practice how to do it and get real-time feedback from a supervisor who is supporting them,” Meyer said. “When they go off campus into their externship sites, we hope that will make them a little more comfortable and a little bit less intimidated by all of the sights and sounds you hear in these settings and also more familiar with the actual types of assessments and tasks they do.”
“It’s exposure they don’t get otherwise,” Shune said.
With an aging population combined with better medical care that allows people such as stroke victims to live longer, demand for graduates of the program is strong and continues to grow. The lab gives students an opportunity to see if they want to pursue a career in acute care or elsewhere in the field instead.
“This is a game-changer,” Shune said. “Some students now see themselves working in this setting. When I was a grad student, I was terrified of acute care. People are sick. There’s a lot of risk in that setting. If we can take away the risk, that’s huge.”
—By Jim Murez, University Communications